Mom Talk: My Ruptured Uterus & Little Soldier Baby
Written by Alyssa Kagel
Photography by Alyssa Kagel
The day before I went into labor with my second child, my mother called to reassure me: “It will be quick and easy this time. My psychic is never wrong.”
I didn’t believe in psychics, but her words comforted me. With this baby, I hoped to avoid the long labor and unplanned C-section that happened my first time around. I wanted a vaginal birth.
I arrived at the hospital nine centimeters dilated, after waiting too long at home for the contractions to reach one minute (they maxed out at 30 seconds). As my midwife conducted her hospital exam, she seemed as confident as my mother that the birth would happen fast. The anesthesiologist had just enough time to administer my epidural. The sound of my baby’s heart beeped on the monitor. The steady baboom-baboom was a comfort as I pushed for three hours with no progress.
Suddenly I felt a searing pain in my stomach, like a band tightening. My body went rigid. I couldn’t speak. The beeping of my baby’s heart slowed without picking up again.
The midwife stared at the monitor, her face scrunched in alarm, and said something on her handheld radio.
“My stomach,” I whispered, sweat dripping down my forehead. The silence between beeps was ominous. “Why is the heart rate so low?”
“Is it a sharp pain all over?” she asked.
I nodded, desperate for the sluggish beeps to quicken. My insides felt like they would explode. I repeated my baby’s name in my head, over and over, like a mantra, suddenly sure it was the right name for him: Miles, Miles, Miles.
My husband and I had discussed the name “Miles” months before his birth, with the help of websites and a detailed spreadsheet. I loved the sound of the name “Miles,” but I was hesitant about the meaning—“soldier.” I thought a name should signify peace, not war. We agreed to decide once we met our baby.
What happened next in the hospital was a blur. The midwife barked more commands into her handheld radio and told me my uterus had likely ruptured. This occurs when a woman’s uterus tears and the baby slides into the mother’s abdomen, unable to breathe. Uterine ruptures are most common in women like me who attempt a vaginal birth after C-section, or VBAC, but the chance of rupture is still low—about 0.5% or 1 in 200; some practitioners say it’s an even smaller percentage.
I tried to digest this news as a gaggle of hospital workers burst into action around me. They snapped on gloves, slid me onto a gurney, murmured amongst themselves, hustled to the operating room. As we sped down the hallway, one of them made a joke for my benefit, probably to distract me. I only recall the strangeness of hearing it, the way I couldn’t lift my lips into a smile. All I wanted at that moment, as my hospital bed rolled down the hallway, was for the baboom-baboom of Miles’s heart to return to normal.
The OR was as I remembered from my first C-section: icy cold, smelling of alcohol, metal tools gleaming. This time everyone dashed around, faces hidden behind masks, working against some invisible clock. My pain continued as a nurse thrust a sheet above my chest, separating my stomach from the rest of my body.
A clipped discussion ensued among the operating staff about my epidural. “Yes,” my midwife said. “She’s had one. But it’s not enough. You need to get in there now. Go with general.”
Someone else insisted they avoid general anesthesia and up my epidural. The latter argument won out. I wanted to tell them to get on with it, my baby might die in there while they argued, but I kept quiet.
My pain finally subsided. Miles’s heart rate slowed further. A doctor sliced me open. The baby emerged minutes after that first cut without making a sound. I learned later that his pulse at birth was 60 beats per minute; the average newborn range is 120 to 160.
“What’s happening?” I asked as nurses and doctors scampered around me. I couldn’t stop shaking; I couldn’t swallow. My baby’s silence repeated into itself.
My husband squeezed my hand. “They’re working on him,” Chris said.
I craned my neck towards the hospital workers and Miles. Even through my hazy, drug-induced confusion, I feared the worst. My husband huddled behind me with a nurse. He wobbled back to my side and sunk into a stool, sipping from a tiny cup of orange juice someone had pushed into his hands.
Later, he told me he’d tiptoed over to the newborn station to ask how our baby was, and the nurse said, “not good.” She lifted Miles’s arm and it flopped down as if he wasn’t alive. Then she rattled off Miles’s abysmal Apgar score—1 out of 10—a test every newborn receives to assess their need for extra care. My husband had almost fainted.
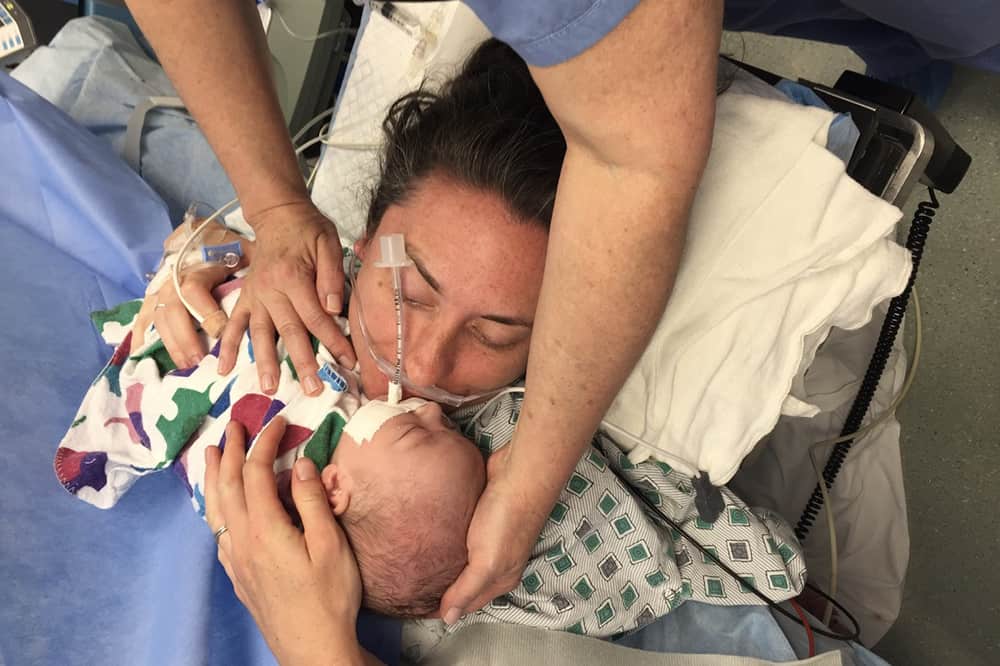
My midwife told Chris to get his camera ready, and she suddenly thrust Miles onto my chest for a photo op. He was wrapped and unmoving, like a newborn doll. He fit perfectly in my arms. I wanted to hold him forever.
“Take a picture, quickly!” the midwife commanded.
My husband obliged, and within seconds Miles was whisked away again. Later, I learned my midwife had convinced the doctors to allow Miles and me that skin-to-skin time in case he died, because at least I’d have the memory. By then Miles’s outlook was still uncertain—though he was finally breathing, he’d gone almost five minutes at birth without taking a breath.
My midwife appeared back at my side and grasped my hand. “We’re doing everything we can,” she said. “We were right, your uterus ruptured.”
“Will Miles be okay?” I asked, searching her face as I lay in the hospital bed.
“We don’t know. He’ll get a helicopter ride to Children’s Hospital. The care is top-notch.”
I stared at her wide-eyed, my heart thumping in my ears. I understood her words to mean: he probably won’t make it.
Someone wheeled me into a recovery room. My husband walked beside me, but it was a lonely trip. I imagined leaving the hospital without a baby, telling my almost-three-year-old that his brother died, fending off awkward condolences from people I hardly knew. I clenched my eyes closed and held my husband’s hand. I’m grateful my husband didn’t share what he’d heard—that Miles’s body would be refrigerated during the helicopter ride to prevent his brain from swelling.
A woman dressed in a white doctor’s coat, who I vaguely recognized as a member of my OB-GYN team, knocked on the door once I’d settled into a recovery room. According to records, the time that elapsed between my uterine rupture and that visit from the doctor—a person who told me the most important news of my life, even though I can’t remember her name—was 30 minutes. It felt like half a life. The doctor’s face appeared neutral as she approached. My body went rigid. I braced myself. At my bedside, she broke into a smile.
“Your baby’s a fighter,” she said. “He’s breathing on his own now. He ripped out the breathing tube himself a few minutes ago, which is an excellent sign. No need for Children’s Hospital anymore—he’ll stay at our NICU.”
My husband and I locked eyes, tears streaming down our faces. I took a deep breath and released my clenched fists.
It was eight hours before the doctors permitted me to see Miles again—I had to prove I was strong enough to journey from my bed to my wheelchair to a seat in Miles’ NICU room. My body had fared well during the birth, with average blood loss for a C-section delivery. Some ruptures require a transfusion.
It’s hard to describe that moment I finally held Miles without evoking clichés about magic and love. I stared and touched and cuddled as I considered an alternate reality in which he had not survived.
Miles and I were released from the hospital three days later, on my husband’s birthday. Our baby had recovered fully within a few hours of birth, but doctors kept him in the NICU during his hospital stay to wean him off his sugar drip. We were relieved—Miles seemed healthy. Except for that little seed of doubt planted by the head nurse as she reviewed our release paperwork with us, noting that Miles showed signs of “high muscle tone” in his lower body.
“Make an appointment with a specialist right away,” she said. “But he’ll probably be fine.”
I turned to Google for diagnosis advice (ill-advised for a nervous parent) and learned that high muscle tone is a sign of cerebral palsy, a group of disorders that affects a person’s ability to move. A baby who doesn’t breathe for an extended period at birth—like Miles—could develop this disorder.
I wasn’t an overprotective parent with my first child, but things changed with Miles. I schlepped him to multiple specialists, monitored every movement and coo. At my second visit with a respected developmental pediatrician when Miles was six months, the doctor looked me in the eye and said, “Your baby is perfectly healthy. You have nothing to worry about.” I heard those words and finally let myself believe my little guy would be okay. It felt like the deep exhalation of a breath I hadn’t realized I was holding in. I shook hands with the doctor, hopeful I’d never see him again.
Miles turned three this July. He blossomed into an inquisitive chatterbox who loves Matchbox cars, M&Ms, and mimicking his big brother. I now focus my energy on parenting two feisty, healthy boys—not thinking about Miles’s birth, or what I would’ve done differently. Life’s too short for that. Surprises will come again, good and bad, though hopefully none as harrowing as my ruptured uterus and all that came with it. When the surprises arrive, I’ll try to soldier on like Miles, who channeled the strength his name embodies to fight for his life from the start. His name is perfect because he’s a fighter. He’s my little soldier.

Are you a mother with something to say? Send us an email to be considered for our “Mom Talk” column.
Write a Comment
Share this story



I came across this post searching for the outcome of healthy pregnancy/deliveries after a uterine rupture and I want to cry over our shared experience. My first (and only child thus far) is also named Miles and we suffered a uterine rupture as well. My Miles also came out quiet and it was terrifying. I also needed a great amount of blood transfusion and we are both lucky to be alive. My son turns 1 this week and each day I’m so thankful for him but also feel so conflicted about having one more. Thank you for sharing your story.